Abortion rights, women of color, and LGBTQI+ people are under attack. Pledge to join us in fighting for gender justice.
Kentucky’s Green Light for Medicaid Work Requirements Threatens Vital Coverage for Women and Families

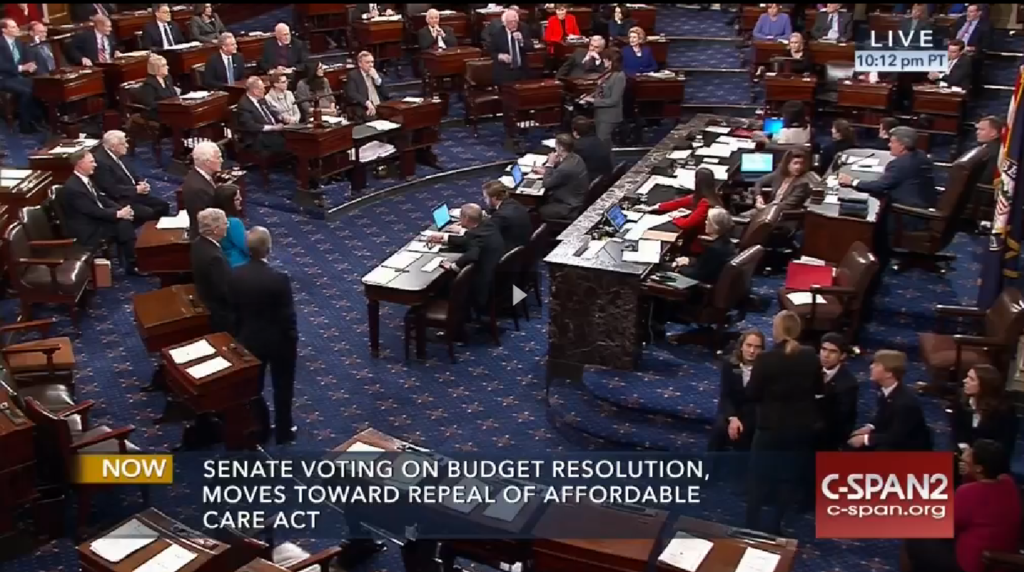
Shortly after the Trump Administration reversed long-standing federal policy by putting states on notice that they could seek to impose work requirements as a condition of Medicaid, CMS announced that it is approving a waiver submitted by Kentucky—one of ten states that submitted a waiver including work requirements. This makes Kentucky the first state in the 52-year history of Medicaid to require individuals struggling to make ends meet—including those caring for relatives, suffering from chronic conditions, or furthering their education—to meet work requirements in order to receive Medicaid coverage. Kentucky’s women will be hit particularly hard by the Administration’s green light to impose punitive work requirements.
Since implementation of the Affordable Care Act (ACA),NWLC estimates show that health insurance rates for women in Kentucky—also a Medicaid expansion state—were above the national average in 2016, with a 17 percent gain in coverage among women in Kentucky just between 2013 and 2016. But, those coverage gains are jeopardized by Medicaid work requirements that force certain enrollees to make the choice between their daily obligations or work requirements—at the risk of losing vital health coverage. And it will undoubtedly be hard for those required to meet Kentucky’s work requirements of up to 80 hours a month. The state also received approval to force people with limited resources to pay premiums or risk being kicked out of the program. According to Kentucky’s own estimates, 95,000 people in the state are at risk of losing coverage under the waiver.
Work requirements go against the very purpose of Medicaid—to ensure that individuals struggling to make ends meet or to manage obligations have access to health care that enables them to do so. That’s why prior requests to create work requirements for Medicaid have been rejected, including as recently as 2016. And for women nationwide—17 million of whom were estimated to be covered by Medicaid in 2016, including 4.4 million women ages 18-64 who NWLC estimates gained Medicaid coverage between 2013 and 2016— the threatened loss of Medicaid coverage due to work requirements is very real.
What is also sickening is the false racialized narrative that underlies the Administration’s “up-by-your-bootstraps” approach to work requirements—the face of which is usually a caricature of an “able-bodied,” single mother of color “collecting” public benefits and willfully refusing to work while living a lavish lifestyle. This false narrative depends on willful disregard of the reality that the majority of individuals enrolled in Medicaid who can work do work—nearly 8 in 10 non-elderly adults enrolled in Medicaid in 2017 live in working families. And this includes many women who work in the health sector in jobs supported by the Medicaid program.
We refute this false narrative—that’s also why we joined with 115 ally organizations in a letter opposing legislative proposals to change Medicaid, including work requirements.
Yet, the Trump Administration and its allies willfully ignore research illustrating the failure of work requirements to lift individuals out of poverty or secure employment when implemented in Supplemental Nutrition Assistance Programs (SNAP) or Temporary Assistance to Needy Families (TANF).
Work requirements create an additional barrier for those unable to meet them and threaten access to vital health care. For women, who already face unequal pay, obstacles to obtaining education, workplace discrimination, and other systemic barriers, the barrier to Medicaid coverage created by work requirements means that both their health and economic security are jeopardized. Women and families struggling to make ends meet need health coverage that enables them maintain their health and economic security. This Administration and its allies should be promoting access to care, not taking coverage away from millions. This dangerous action, based on a false racist premise of Medicaid enrollees, will wreak very real harm on the health and economic security of millions of women and families.