The National Women’s Law Center fights for gender justice—in the courts, in public policy, and in our society.
New Medicaid Bulletin Highlights Innovative State Birth Control Policies
There’s a lot of talk these days about the promise of intrauterine devices (IUDs) and implants, often referred to as long-acting reversible contraception (LARCs). States, including Delaware and Colorado, are committing to improving access. Studies are showing women choose LARCs when they learn more about them and they are easily accessible, including being made available without financial barriers. Indeed, more women in the United States are choosing these “set it and forget it” birth control methods than ever before – with the latest data showing 12% of women who use birth control choose an IUD or implant. But it seems that there is a gap between the number of women who want an IUD or implant and the number of women who actually get one. There are a number of reasons for that gap, but a major one is that it has been challenging for health care providers to get compensated by insurance companies for providing this care, which can be expensive.
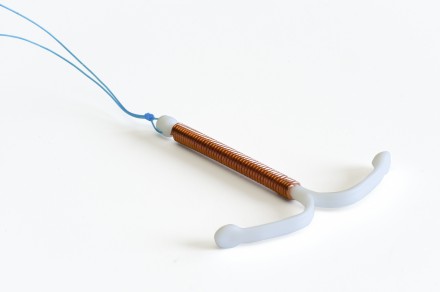
If you’re thinking, “I thought doctors make a lot of money. Should I really be concerned with health care providers getting paid by insurers?” Yes, you should be concerned. If a health care provider isn’t compensated, it becomes difficult for them to provide care to their patients, and in turn makes it harder for patients to get the care they need. That’s a real problem. However, just last week the Center for Medicaid and CHIP Services (CMS) released an informational bulletin highlighting ways that states have improved access to IUDs and implants in their Medicaid programs by developing new approaches to how health care providers get paid. Many of the states featured in the bulletin have taken steps to ensure that women covered by Medicaid who want an IUD or implant after they have a baby are able to get one before they leave the hospital or birth center.
Why is this so important? Because women who want an IUD or implant after delivering a baby often have to wait until a follow-up appointment to get it. This isn’t because it’s unsafe to get it right after delivery, but because of the way the costs of labor and delivery are billed. Sometimes there is no way for Medicaid to pay the hospital or health care provider for the IUD or implant and its insertion, which means the provider can’t provide that service. A woman in this situation then leaves the hospital without her birth control method of choice until a follow-up appointment six weeks later. Unfortunately, many women don’t make it to that follow-up appointment, particularly women who have little advance notice of work schedules, who rely on public transportation, or who don’t have child care. As CMS highlighted in the bulletin, some states have changed the way the billing system works to ensure women can get an IUD or implant at the same time as delivery, thus ensuring women have their birth control method of choice when they need it, reducing the chances of unintended pregnancy.
The bulletin doesn’t change Medicaid policy per se, but it does indicate that CMS approves of the innovative policies. Hopefully more state Medicaid programs will see these innovations as opportunities they could also undertake to improve women’s access to LARCs. And with birth control access so strongly linked to women’s greater educational and professional opportunities and increased lifetime earnings, these innovations have the potential to improve not only women’s health but also their economic security.